On April 8th, 2024, a total solar eclipse will sweep across North America, from Mexico to the Maine-Canadian border. For those who experienced the spectacular solar eclipse of 2017, this one will be similar, crossing the United States from west to east and passing...
Getting stranded in a violent storm can be extremely dangerous. Often, all you can do is hope the storm will abate before streets flood and buildings collapse. The same is true of a cytokine storm, a squall that rages inside your own body as an overreaction to infection, injury or other stimuli. Here, we will take a look at these cytokines, the story of how they were discovered and how physicians can control cytokine storms to treat health conditions ranging from arthritis to COVID-19.
Cytokines are like emails: they are small proteins that form an intricate communication network among the cells of our body. To date, scientists have identified dozens of different cytokines that perform a vast range of functions, from contributing to the success of a pregnancy to influencing the structure of our bones, and many more. However, cytokines are mostly known for regulating your immune system. One type of cytokines called pro-inflammatory cytokines induce inflammation, one way your body responds to injury or infection. Unfortunately, inflammation can turn from protective to dangerous, and even lethal, when it goes uncontrolled. Consequently, pro-inflammatory cytokines can cause extreme damage to cells and tissues. For example, cytokines can cause blood vessels to leak, causing the surrounding tissue to swell. If that swelling is in the airways of the lungs, it will make it difficult to breathe, and if it’s in the brain, it will cause neurological damage.
Because they can be so dangerous, your body tightly regulates the production and function of pro-inflammatory cytokines. For example, anti-inflammatory cytokines counteract pro-inflammatory cytokines. Your body also produces inhibitors, or molecules that block the activity of specific cytokines.
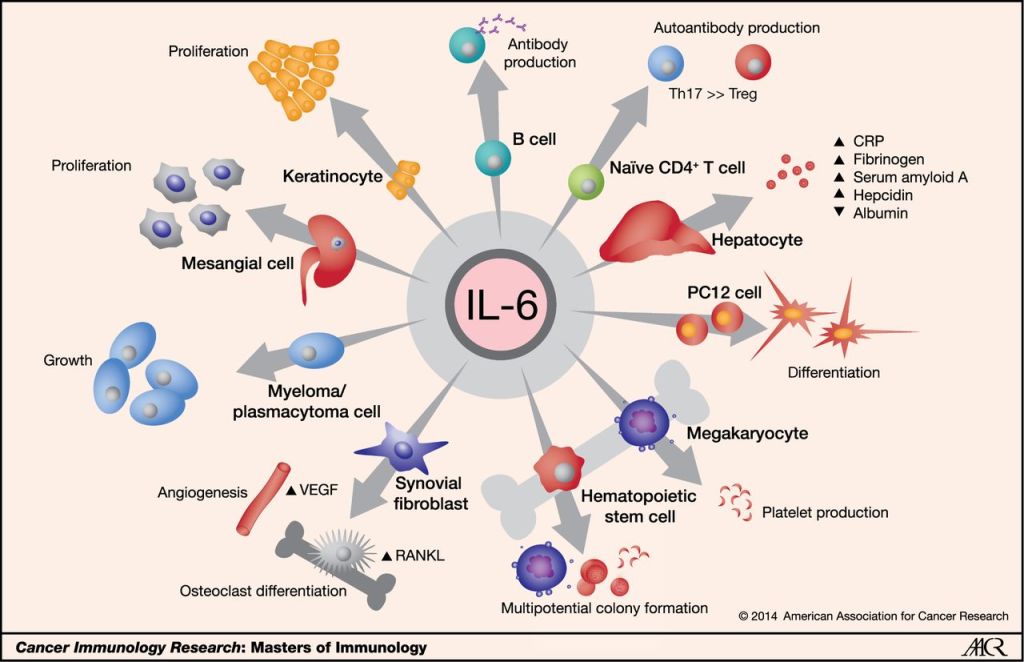
The research that led scientists to identify pro-inflammatory cytokines began in unexpected places: Several research groups were simply trying to understand a wide variety of seemingly unrelated phenomena in the body. For example, some research groups were trying to pinpoint the molecules that cause fever in response to an infection. Other groups were trying to determine what causes bone and cartilage damage in people who have arthritis. A third set of investigators was trying to figure out what regulates the growth of a type of immune cell. As scientists continued to explore these questions, they were surprised to discover that the two twin proteins – later named IL-1 alpha and IL-1 beta – were responsible for all of these processes. Yet another group of researchers was exploring the changes that take place in the liver during an infection, as well as the function of another type of immune cells called B lymphocytes. It turned out that a protein very similar to IL-1, called IL-6, was the key to both of these processes. These studies helped us find the first members of what we’d later find out is a large family of pro-inflammatory cytokines.

The discovery of pro-inflammatory led us to overturn several common scientific beliefs of the time. For example, when scientists identified IL-1, IL-6 and other cytokines, they realized that the symptoms of an infection are caused not by microbes but by our own immune systems in response to the presence of microbes. (But don’t worry: while these cytokines literally make us feel sick, they are also essential in directing the immune system to control the infection.)
We also learned that we could control cytokines as a form of therapy. For example, when scientists discovered that cytokines are responsible for inflammation, this meant big changes were coming in the treatment of inflammatory conditions such as rheumatoid arthritis, inflammatory bowel disease and psoriasis. Researchers began developing drugs that treat these conditions by mimicking the natural cytokine inhibitors in the body.
But while these medications are effective at relieving symptoms of these chronic conditions, they also come with side effects. Since cytokines play a central role in regulating the response to germs, inhibiting them can increase one’s risk of certain infections.
Scientists are now exploring whether blocking cytokine activity can relieve the most severe symptoms of COVID-19 — those that are caused by cytokine storms, in this case, high levels of IL-6. Indeed, scientists have found that patients with a severe case of COVID-19 have higher blood levels of IL-6 than patients with a mild case. Now, some institutions have launched clinical trials to assess whether inhibiting IL-6 benefits patients with cytokine storms caused by the virus. While we await the outcome of the trial, it’s important to remember that although blocking cytokines might stop the dangerous inflammatory storms associated with COVID-19, it may also prevent the immune system from effectively fighting the virus.

Just like rain can be beneficial during a drought but can create havoc when it turns into a violent, destructive storm, our bodies need cytokines to tame infections but, these same cytokines can become dangerous and lethal when they start acting out of control. Thus, when developing therapies, scientists need to figure out ways to manage the delicate balance between the beneficial and detrimental sides of cytokines. As scientists implicate cytokines in more and more diseases, ranging from heart disease to obesity to depression, it’s becoming even more important to figure out how to control these molecules. Who knew that researchers who were merely trying to understand how our bodies work would find the cause of so many health issues? This just goes to show how important basic research is: it’s worth seeking answers to questions, even when we don’t know where the research is going to bring us, because it might lead to the discovery of something critical to our health and well-being.