On April 8th, 2024, a total solar eclipse will sweep across North America, from Mexico to the Maine-Canadian border. For those who experienced the spectacular solar eclipse of 2017, this one will be similar, crossing the United States from west to east and passing...

Imagine drinking ten glasses of sugar water. What would you do after? Wash out your mouth? Eat something salty? You’d probably eat or drink whatever it takes to get rid of the extremely sweet taste. In the same way, when your body encounters high blood sugar, it tries to lower your glucose back to normal levels. Insulin, meaning island in Latin, is a hormone that is made in your pancreas. Its primary role is to reduce your blood sugar. Defective insulin secretion, which is the hallmark of diabetes, can have adverse consequences in the body, such as unintended weight loss, increased thirst, increased urination, vision problems, and skin problems.

Diabetes in the United States. Type 1 is usually caused due to a family history. Although there is no way to prevent it, the treatment includes taking insulin injections and maintaining a healthy lifestyle. Type 2 diabetes may be linked to family history, excess body weight, and an inactive lifestyle. The treatment is similar to type 1 diabetes. Image credit: Joint Base San Antonio & Centers for Disease Control and Prevention.
The History of Insulin and Blood Sugar
While insulin is now recognized as essential to the body’s everyday function and millions of people take insulin injections to treat diabetes, this understanding wasn’t always so clear. The source of insulin was discovered in 1869 by Paul Langerhans, a German physician who was studying the structure of the pancreas. He observed that there were clusters of cells scattered throughout the pancreas, which he named the islets of Langerhans. For the next two decades, the scientific community tried to understand how these islets worked. Since these types of experiments would be unethical in humans, to study the pancreatic islets, scientists instead removed the pancreas from healthy dogs. What they discovered was that as a result sugar appeared in the dogs’ urine. This was a sign that the pancreas is involved in regulating the body’s glucose levels. These studies began to establish the link between the pancreas and diabetes. Today, doctors test for glucose in urine as a diagnostic marker for diabetes.
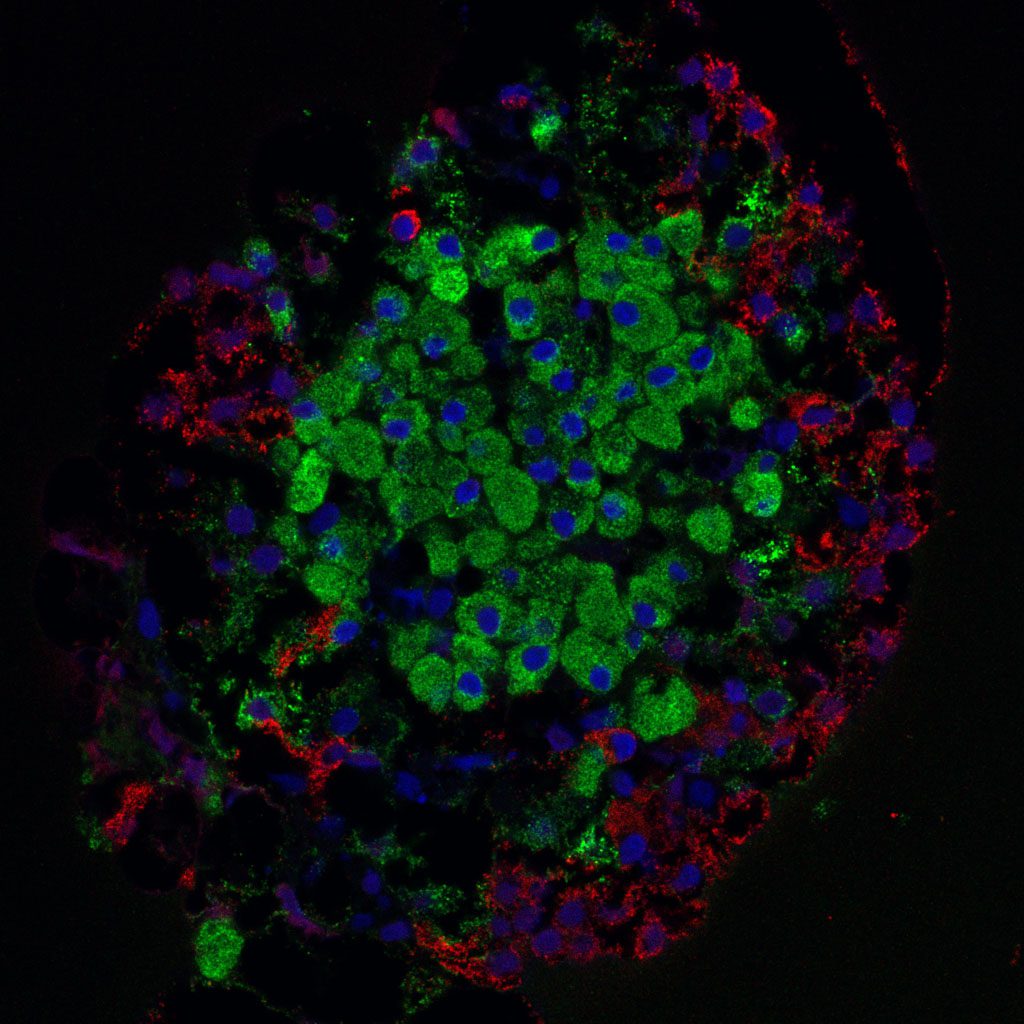
Section of a rat pancreas showing the islets of Langerhans as viewed under a microscope. The cell nuclei have been stained blue, the cells that secrete insulin have been stained green, and the glucagon secreting cells have been stained red. Glucagon is a hormone that is released when the insulin levels are too low, and it increases the sugar concentration in the blood. Image credit.
Synthetic Insulin for Controlling Blood Sugar
The next step in research was to produce insulin in order to treat diabetes, however this proved to be an uphill task that took another three decades. The delay was partly because of World War I and partly because insulin is sometimes damaged by enzymes in the digestive system, making it difficult to extract. In 1920, Sir Fredrick Banting, a Canadian physician, realized that cutting the blood supply to the pancreas would destroy all of the cells except the islets. Upon isolating these cells, insulin could now be successfully extracted. Banting and Charles Best, another Canadian scientist who worked as an undergraduate student with Banting, took the insulin they extracted and injected it into a diabetic dog. The extract reduced the blood sugar levels by 40% within an hour.
Banting presented his findings to J. R. R. Macleod, a Scottish biochemist, who provided him with funding and a better equipped lab. Banting then transitioned from working on dogs to working on fetal calves, as the process of extracting the insulin from the calves was much less time consuming than in dogs. Furthermore, the calves had not yet developed the other digestive glands, so the insulin was at less of a risk of being damaged by other enzymes. Although the technique was successful, the extract still contained a large number of impurities. Eli Lilly and company offered to help Banting and Macleod, and together they manufactured the first highly refined insulin, which was made available to the general public shortly after 1921. Banting and Macleod were awarded with the Nobel Prize in Physiology in 1923 for their work on insulin.

An advertisement for insulin from 1929.
Problematically, using insulin from animals has the potential to cause allergic reactions in some individuals with diabetes. It became necessary to find a way to synthesize human insulin in large quantities. The advent of techniques that could genetically manipulate DNA in various organisms led to the synthesis of genetically engineered human insulin in the bacteria E. coli in 1978 and circumvented the problems with allergic reactions to animal-based insulin. The effort was funded by Genentech and led by three scientists: Arthur Riggs, Keiichi Itakura, and Herbert Boyer. In 1982 the biosynthetic human insulin or “Humulin” became commercially available.
The World Health Organization has predicted that over the next 20 years insulin sales will grow from $12 billion to $54 billion annually. Although individuals with Type 1 and individuals with Type 2 diabetes both require insulin, late stage Type 2 diabetes requires higher doses because of the development of insulin resistance in these individuals. Individuals with Type 2 diabetes may produce enough insulin, but their cells become resistant to the effects of insulin: the cells block glucose from entering to be metabolized, so glucose stays in the bloodstream, causing your blood sugar to rise.
The Future of Diabetes Care
To counter the rising costs of care, scientists are developing gene therapy approaches to actually cure diabetes. The first approach targets Type 1 diabetes and involves administering proteins which can reprogram some pancreatic cells that synthesize glucagon to synthesize insulin instead. The second approach involves administering a hormone that causes weight loss, which in turn reduces insulin resistance and thus reduces the effect of Type 2 diabetes. Both studies have been carried out in mice, which are used as models for diabetes before testing treatments in humans. The next step will be to test these procedures on larger animals and ultimately in humans in clinical trials. If these trials are successful, we will be one step closer to extinguishing diabetes.