On April 8th, 2024, a total solar eclipse will sweep across North America, from Mexico to the Maine-Canadian border. For those who experienced the spectacular solar eclipse of 2017, this one will be similar, crossing the United States from west to east and passing...
“It’s just like having a bad case of the flu.”
“It can kill you.”
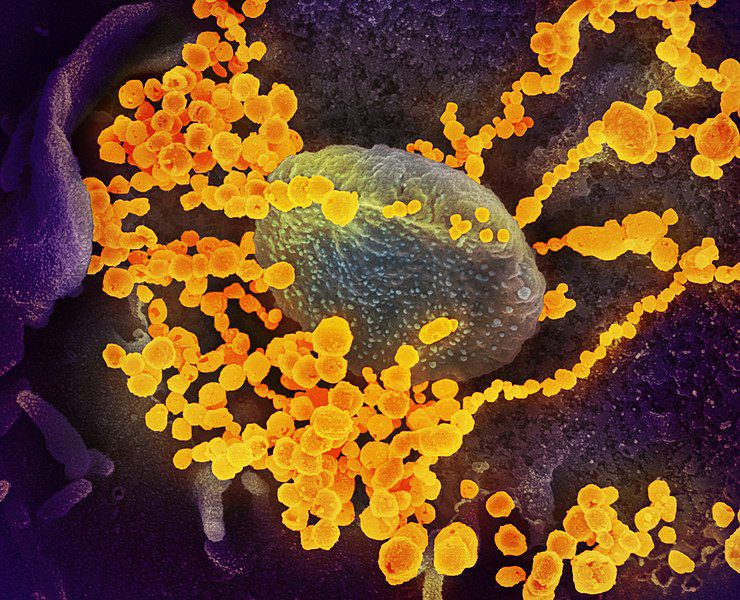
You’ve likely heard both of these statements in conversations about COVID-19. While the severity of the disease was a common point of disagreement in early discussions about how we should respond, it’s now apparent that both statements can be true at once. Some people who get infected with SARS-CoV-2, the virus that causes COVID-19, only have a mild disease, while others develop a life-threatening condition. How can this be? The way in which each person’s cells respond to the viral infection is a major element in explaining the many faces of COVID-19.
When viruses like SARS-CoV-2 enter our body, they can only reproduce if they are able to reach the inside of a cell. Once inside the cell, the virus hijacks the cell’s reproductive machinery to replicate its own genetic material. These copies are then packaged into particles that leave the cell and go on to infect other cells in the body. When a person speaks, sings, coughs or sneezes, they release this material into the environment, where it can infect other people.

A virus is sneaky, but when it enters a cell, it doesn’t go unnoticed. Cells have sensors that detect the presence of viruses. Once these sensors are activated, they set in motion a series of molecular events that help the body defend itself. One of the most important actions an infected cell takes is to alert its neighbors of the virus, giving them time to prepare. This alarm bell comes in the form of a family of small proteins: interferons.
If all goes well, the interferon system helps prevent spread of the virus to other cells. By communicating with immune cells, interferons can also help the immune system step up its game in anticipation of fighting the virus.
While evolution has endowed cells with the ability to warn each other about a virus using interferons, it has also pushed viruses to forge strategies that interfere with the cell’s alert system. And because viruses reproduce so quickly, they have more opportunities to make changes that will help them evade the body’s response. Viruses are very good at adapting to the cell’s response in ways that allow them to thrive.
Some viruses, like SARS-CoV-2, try to prevent an attack by the body at every turn. These viruses have evolved the ability to hide from the sensors that trigger a cellular response. Even if they cannot manage to go completely undetected by the cell they are infecting, they can impede the series of molecular events that allows that cell to produce interferons. And, should the infected cell still be able to circumvent the virus’s strategies and manage to produce interferons, these viruses can still dampen the alert delivered to other cells. Some viruses have even gone so far as to steal genetic material from the cell to make their own anti-interferon proteins (fortunately, it looks like we don’t have to worry about this counterstrategy when it comes to SARS-CoV-2).

Our cells’ ability to properly respond to viruses—and a virus’ ability to adopt strategies that counteract that response—is not just a source of endless fascination for molecular and evolutionary biologists, virologists, immunologists and geneticists. These activities also have real-world consequences, as they can determine the severity of a viral infection.
In COVID-19, a person’s response to the virus is heavily tied to the activity of their interferons.
People with reduced production of or a reduced response to interferons have a harder time clearing the virus from their body and tend to show more intense symptoms compared to people who produce and respond to interferons in appropriate ways. Additionally, some individuals produce another type of immune protein called auto-antibodies that attach to the interferons and prevent them from functioning. These individuals are more likely to have severe disease compared to people who do not make these auto-antibodies. Interestingly, these individuals are almost exclusively men, who, incidentally, experience more serious COVID-19 symptoms compared to women. The interactions between SARS-CoV-2 and the interferon system may even help explain some of the health disparities that are present among different groups of people. For example, there is evidence that the stress associated with oppression, discrimination and racism may affect interferon activity and lead to more severe COVID-19 disease in people of color.
Since interferons are so important in mediating viral infections, they might one of the keys to treating them. For example, one type of interferon was once the therapy of choice for individuals with hepatitis C. While more effective medications are now available to treat hepatitis C, scientists are currently evaluating injections of interferons as a potential treatment for COVID-19. The jury is still out on whether interferon has any effect, as one major study where interferon therapy showed no benefit in individuals with advanced disease has been discontinued. However, researchers are still evaluating whether injections of interferon can work in the initial stages of COVID-19. Regardless of the outcome of this work, it’s clear that the molecular mechanisms at the heart of basic research are making a concrete difference in our understanding of—and potentially our ability to treat—viruses like COVID-19.