On April 8th, 2024, a total solar eclipse will sweep across North America, from Mexico to the Maine-Canadian border. For those who experienced the spectacular solar eclipse of 2017, this one will be similar, crossing the United States from west to east and passing...
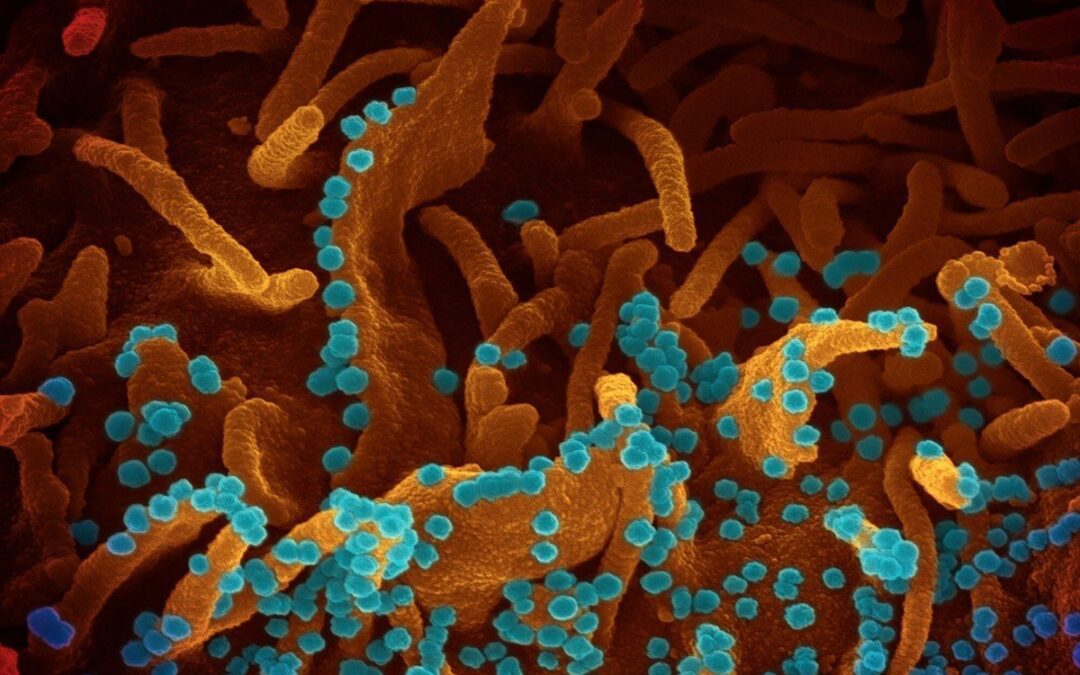
It’s been about year since the novel coronavirus SARS-CoV-2 (COVID-19) began spreading in the U.S., leaving many people with a firm understanding of what this “new normal” looks like. Awkward social distancing slip-ups, mask acne, and quarantine cabin fever are integrated into our current consciousness— alongside news of skyrocketing COVID infection numbers from your latest doom-scrolling session. The pandemic incited scientists and doctors to publish hand-over-fist on the short-term symptoms of COVID-19 infection. As a whole, the research community scrambled to understand the virus and flatten the curve, focusing on surviving the challenges at hand.
The immediate effects of the virus presented with common symptoms of infection like fever, cough, loss of taste or smell, and a sore throat. Surprising, however, was the onset of stroke cases in young (30s and 40s) COVID-19 patients, alongside reports of brain hemorrhaging and memory impairment. These phenomena sparked scientific studies of the impact of COVID-19 on the brain, which showed that the virus could infect the brain’s nerve cells, called neurons, and kill them. The virus can enter a neuron through a doorway into the cell called the ACE2 receptor. This receptor is located on the surface of cells and is found all over the body. Though ACE2 does not appear as often in the brain, it is found in neurons inside the hippocampus, a sea horse-shaped structure that plays an important role in learning and memory. Some COVID-19 patients experience memory loss, which may be explained by the virus infiltrating hippocampal neurons through the ACE2 receptor.
Scientists think that the coronavirus may turn neurons into “zombie cells” that are technically alive, but do not go through the cell cycle to grow and divide. When a cell detects the viral invader, it may revert to zombie mode to prevent the virus from using the cell as a tool for replication. It’s a brilliant defense mechanism, but it becomes dangerous as the zombie cells begin to release molecules that cause inflammation. This contributes to what researchers have deemed “inflamm-aging”, when chronic inflammation damages your brain cells, causing lasting effects that you’d typically see in older populations, such as memory loss. Dr. Kevin Hascup, an Assistant Professor at Southern Illinois University, says, “The question becomes once the virus enters the brain, what is it doing? … If it is permanently stopping the cell cycle, this could have much longer-term implications than just the duration of the virus in the body.”
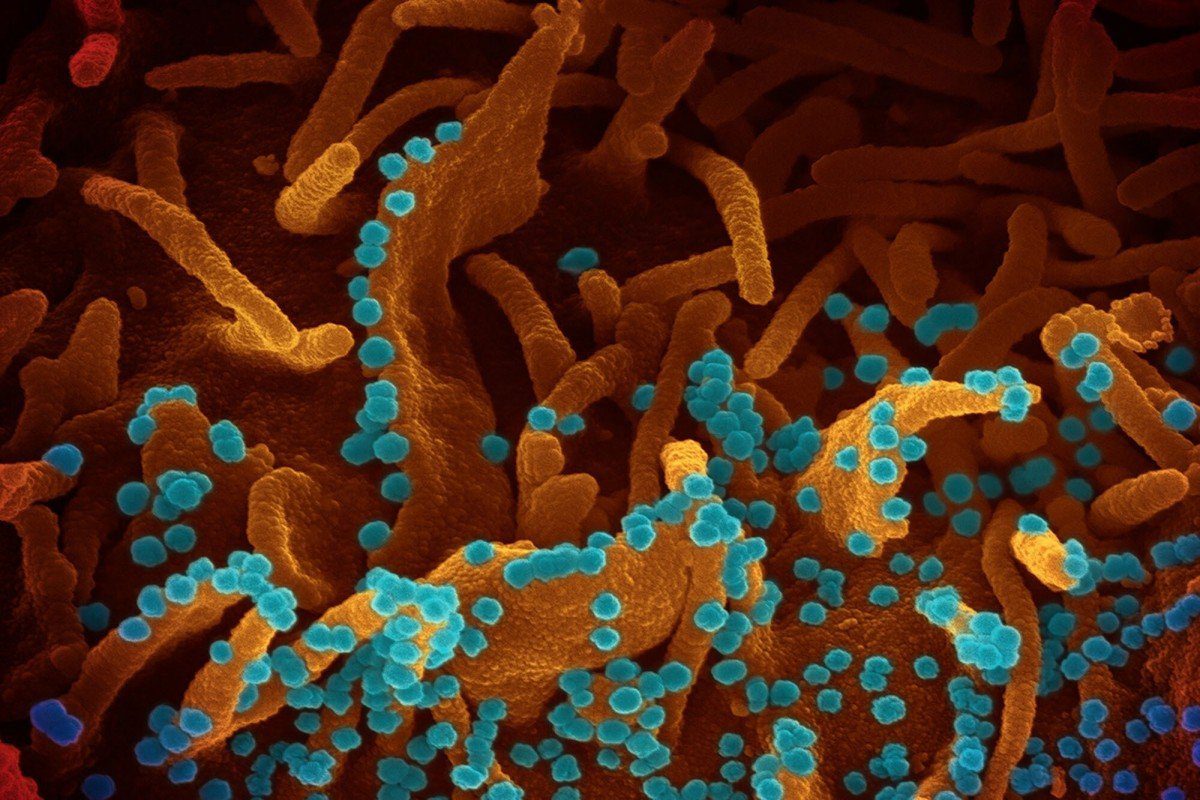
Indeed, the neurological symptoms arising from a coronavirus infection may have consequences that outlast the virus. Sure, the COVID “brain fog” of headaches, anxiety, and other symptoms will dissipate with recovery. However, researchers warn that the more serious symptoms, like inflammation and strokes, could lead to psychiatric conditions, cognitive decline and other permanent neurological damage. Additionally, some researchers indicate that viral infection of the brain may accelerate the cognitive aging process. However, we need to wait and do more research over time to assess whether this claim is true.
Unfortunately, the populations that are already experiencing deteriorating brain health—the elderly and patients suffering from progressive neurodegenerative diseases like Alzheimer’s disease (AD)— are most susceptible to viral damage to the brain. Research suggests that older patients are at greater risk of the virus entering the brain because of a weakened blood-brain barrier (BBB). This tightly packed layer of cells acts as the gatekeeper to the brain, preventing harmful toxins and pathogens from entering. Dr. Hascup describes “’leaky parts’ in the BBB where the virus can get into the brain…, which occurs faster in AD patients than in normal healthy aging patients.” Viral penetration of a compromised BBB poses a huge risk for infection of the central nervous system, leading to activation of the brain’s innate immune response and eventually inflammation of the brain. This is not ideal, particularly for a disease that already sees a substantial amount of brain inflammation from its own pathological interworking. Even worse, the inflammation generated from viral infection and the build up of zombie cells can further weaken the BBB, creating a cycle of perpetual damage to the brain.
Researchers who study the aging process fear that COVID-19 poses a huge risk to long-term health, though the extent and nature of this risk remain uncertain. Accumulation of zombie cells and inflammation serve to accelerate the process of brain aging and potentially worsen the symptoms of preexisting neurodegenerative disease. As the elderly population swells with each passing year, future studies through time will uncover the lasting damage of contracting COVID-19 on this community.