On April 8th, 2024, a total solar eclipse will sweep across North America, from Mexico to the Maine-Canadian border. For those who experienced the spectacular solar eclipse of 2017, this one will be similar, crossing the United States from west to east and passing...
You’re sitting in a room at your doctor’s office. Today, you might be visiting for a checkup. Or perhaps you simply need a prescription refill. No matter the reason for visiting, you most likely will be asked, “Would you like a flu shot today?”
Vaccines are surrounded by controversy with opposing sides certain they are giving patients the truth. But have no fear, your answer is near. To help you decide whether you’d like a flu shot this season, this article will cover the flu vaccine from conception through injection.
Do I really need a flu shot?
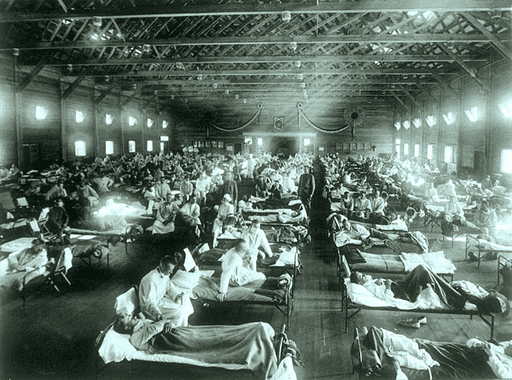
Whether you’ve caught it or not, you’re probably well acquainted with the flu and the virus it is caused by, the influenza virus. The flu, characterized by fever, body aches, coughing and sneezing, is often considered a miserable inconvenience but if we look back at history, we quickly realize these infections can be deadly. In 1918, this virus caused the deadliest pandemic in modern history, infecting 500 million people worldwide and killing as many as 50 million.
Since then, influenza virus has created three more global outbreaks – the most recent one taking place in 2009. Even though influenza activity in the Northern hemisphere is lower compared to other parts of the world, the United States is not immune to this virus’ mayhem. In the most recent data available, influenza and pneumonia is ranked as the eighth leading cause of death in the U.S.
Influenza is a highly contagious virus, making its home in an infected person’s nose, throat, and sometimes lungs. The virus searches for new hosts on the backs of droplets from coughs and sneezes, traveling a shocking 6 feet from its source. This is partially why infected persons are asked to stay home – to avoid passing the flu to others. For most, the illness is mild and resolves in less than two weeks without medical intervention. But others are hit harder by influenza infections.
Young children, pregnant women, and the elderly over 65 years of age are at a higher risk for developing flu-related complications, such as pneumonia, that can result in hospitalization or death. Catching the flu is also dangerous for individuals with chronic health problems, ranging from asthma and heart disease to extreme obesity. Individuals at high risk are especially urged to get the flu shot as their best protection against influenza and influenza-related complications.
What does the flu vaccine do?
A vaccination gives the immune system a leg up against pathogens. The flu shot consists of inactivated (killed) or weakened virus, providing your immune system with a sketch of influenza and arrest warrant against it. The immune system is responsible for not only recognizing the presence of a foreign invader, like influenza, but also for mounting a defense against it.
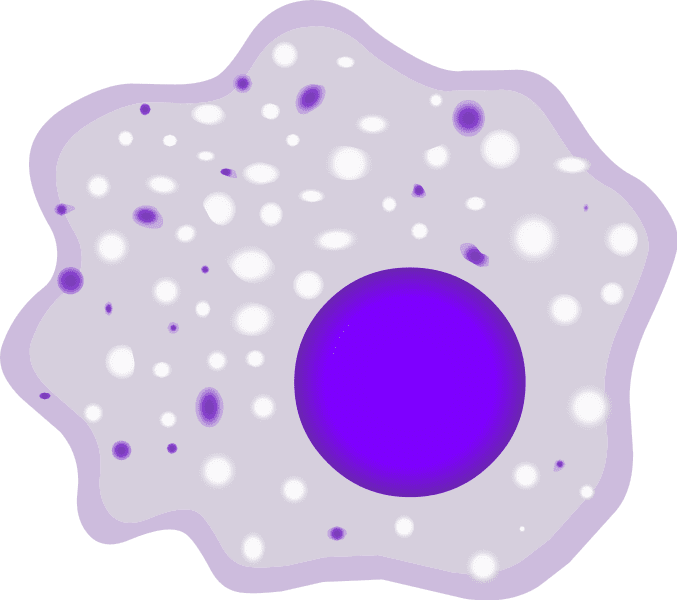
Our body’s defense system is extensive. It is made up of many different cell types, like the different branches of law enforcement – and they are all on the lookout for pathogens. There are three main cell types involved in the body’s response to a vaccination: macrophages, B cells, and T cells. Macrophages are like squad cars on patrol, circulating through the body via blood vessels and entering into tissues if trouble is detected. When macrophages spot the inactivated or weakened influenza from the flu shot, they arrest it, literally gobbling it up. Macrophages then present chewed-up fragments of fugitive influenza to their bosses, T cells.
T cells are called to action after running into a macrophage that is presenting influenza. It’s like local law enforcement calling in the feds. T cells, in turn, respond to the macrophage alert by sending a chemical message to help activate the big guns, B cells.
B cells have two major roles following a flu shot. Their first job is to produce highly specialized proteins called antibodies, which act like a task force. This task force is specific, recognizing only a unique and specific site on the surface of the pathogen that triggered their production. Antibodies circulate throughout the body hunting for the flu virus. Once it’s found, antibodies swarm the virus, neutralizing it on the spot.
The second task of B cells after a vaccination is keep “immunological memory.” Memory B cells are essentially the body’s “Most Wanted” list – they spend the rest of their existence circulating through the body, keeping watch for when influenza attempts to sneak in again. When that time comes, they spring into action and are even more effective than when they first encountered the flu virus. Immunological memory is not unique to B cells – T cells also form memory cells, and these are responsible for seeking out and destroying infected cells should influenza escape from macrophages and antibodies.
The flu vaccine creates a training scenario for your immune system. It attempts to imitate infection so your immune system can build up the resources it needs to fight off a real infection.
Are flu shots safe?
Google the words “are flu” and the above question is the first suggested search. Undoubtedly, fear of adverse side-effects is a driver of low vaccination rates.
The side effects from the flu vaccine are generally mild. They include redness, swelling, and soreness at the injection site. Contrary to popular belief, you cannot get the flu from the vaccination. This is because the vaccine is made with either inactivated influenza virus or influenza virus weakened to the point it cannot cause illness.
A frequently voiced concern with flu shot safety centers on one of its ingredients: thimerosal. Thimerosal is a mercury derivative added to the vaccine as a preservative, preventing harmful bacteria and fungi from contaminating it. Mercury is toxic in high doses, but thimerosal is a mercury-containing compound, not mercury in its pure form. Also, thimerosal is present in a flu vaccine in concentrations of about 0.01%, which is about the same amount of mercury found in a three-ounce can of tuna fish. If you’re still worried, there’s a solution. Simply request a thimerosal-free flu shot.
Let’s be clear – the flu vaccine can cause harm in a small group of people. This includes children under 6 months of age and individuals with life-threatening allergies to any vaccine ingredients. The Centers for Disease Control and Prevention (CDC) also recommends those with a history of Guillain-Barre Syndrome, a rare nerve disorder, consult their doctor before getting a flu shot. Everyone else has the green light to get vaccinated.
Those that cannot take vaccines for health reasons rely on the health of their community to avoid the flu through a phenomenon called herd immunity. When a large percentage of the population (a “herd”) is immune to influenza, those that lack immunity are indirectly protected. This is because influenza cannot find enough permissive noses and throats to grow in.
Achieving herd immunity truly requires a communal effort. A recent study estimated that 80% of healthy individuals and 90% of high-risk persons in the United States need to be vaccinated to establish herd immunity.
Are flu shots effective?
On a good year, 60% of those that get the flu vaccine will frolic through flu season without infection. In a bad year, as few as 10% of the vaccinated will be protected. But this isn’t just because vaccines themselves are sometimes ineffective. It’s also because influenza is hard to characterize, and it is difficult for vaccine developers to identify the correct target to go after.
Influenza virus is difficult to characterize because it mutates rapidly, making subtle variations in the regions of the virus that the immune system produces antibodies against. It’s like the virus is altering its appearance so it can’t readily be recognized on the “Most Wanted” list.
Because influenza virus is constantly changing, the flu shot has to be adapted every year. However, the current procedure to formulate the flu vaccine takes about half a year. As a result, the flu may have already mutated by the time the vaccine is ready, resulting in poor protection. But scientists are discovering the problems with efficacy are more complicated than making ill predictions.
Time to Roll Up Your Sleeve
“Would you like a flu shot today?”
It’s decision time.
Perhaps you’re pregnant or just had a baby and you want to do all you can to protect the little one from the flu. Maybe you take the flu jab to help protect those who can’t get vaccinated.
No matter your reasoning, annual flu vaccination is your best bet for protecting yourself from the flu, flu-related complications, and spreading influenza virus to a loved one at high-risk.
Ultimately, it’s up to you, but I only urge you to ask yourself, “Why not?”
Laura Rughe is a Ph.D. candidate in Microbiology and Immunology at Northwestern University. You can follow her on Twitter @llruhge.